Abstract
Lysyl oxidase (LOX) is a copper-dependent monoamine oxidase whose primary function is the covalent cross-linking of collagen and elastin in the extracellular matrix (ECM). However, the regulation of LOX activity in renal fibrosis is not well understood. Here, our study showed that (a) LOX expression and ECM cross-linking were markedly increased in fibrotic kidneys. Reduction of copper levels in the Golgi apparatus by treatment with the copper chelator tetrathiomolybdate or by specific knockdown of copper transporter 1 (CTR1) decreased LOX activity and ameliorated renal fibrosis. (b) Overexpression of ATP7A caused an elevation of copper ions within the Golgi apparatus, resulting in increased LOX activity and enhanced ECM crosslinking, thereby promoting the progression of renal fibrosis. Knockdown of ATP7A showed the opposite result. (c) FBLN4 was essential for the ATP7A-mediated transfer of copper to LOX and formed a ternary complex of ATP7A-FBLN4-LOX. Our research revealed that high ATP7A expression induced copper overload in the Golgi apparatuses. FBLN4 then assisted ATP7A in transporting this excess copper to LOX, resulting in LOX overactivation. This, in turn, catalyzed the cross-linking of ECM components, thereby accelerating renal fibrosis.
Authors
Wenqian Zhou, Yan Zheng, Yuqing Liu, Jing Liu, Yiguo Liu, Yangyang Niu, Ying Yu, Xiaoqin Zhang, Yingying Zhang, Chen Yu
Abstract
Cystic fibrosis (CF) is a life-limiting genetic disorder caused by deleterious variants in the CFTR gene that results in altered mucus impairing the airway epithelia. Durable correction of these variants in airway cells remains a therapeutic challenge for about 10% of individuals unresponsive to CFTR modulators. A common disease-causing CFTR splice site variant, 3120+1G>A, was corrected in primary CF airway cells using base editor RNAs. Single-cell RNA sequencing revealed a remarkable increase in detectable CFTR transcript in most CF airway epithelial cell types resulting in notable enrichment of CFTR-expressing ionocytes and secretory goblet cells. Progenitor basal cell subtypes were edited, but they decreased as a fraction of total cells and CFTR-expressing cells compared with unedited cells. CRISPR base editors delivered by polymeric nanoparticles (PNPs) facilitated functional rescue of CFTR to clinically meaningful levels in immortalized and primary airway cells. PNPs delivered GFP-encoding RNA to progenitor airway cells in fully differentiated airway cultures. Vitronectin was a major component of the PNP corona that formed in vivo, but preincubation with vitronectin did not enhance delivery. Together, these findings validate a scalable, nonviral platform with compelling translational promise for treating CF and other respiratory diseases involving respiratory epithelial cell dysfunction.
Authors
Erin W. Kavanagh, Anya T. Joynt, Audrey R. Pion, Alice C. Eastman, Alianna I. Parr, Katherine L. Starego, Manav Jain, Sydney R. Shannon, Edwin J. Yoo, Gregory A. Newby, Stephany Y. Tzeng, Neeraj Sharma, Jordan J. Green, Garry R. Cutting
Abstract
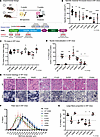
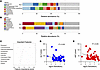
Centronuclear myopathies (CNMs) are rare congenital disorders characterized by muscle weakness, fiber hypotrophy, and organelle mislocalization. Most cases arise from mutations in MTM1 or DNM2, encoding myotubularin and dynamin-2, respectively. DNM2 is a GTPase that binds lipids, oligomerizes around membranes, and mediates fission. We previously showed that DNM2 levels are elevated in MTM1-CNM patients and Mtm1–/y mice, and that normalizing DNM2 rescues disease phenotypes. However, the specific DNM2 functions driving pathology remain unclear. Here, we expressed AAV-delivered WT and DNM2 mutants in WT and Mtm1–/y mouse muscles to disrupt specific DNM2 molecular functions. In WT mice, overexpression of WT DNM2 and most mutants induced CNM-like phenotypes, including reduced force, fiber hypotrophy, and centralized nuclei, consistent with gain-of-function mechanisms. The lipid-binding-defective mutant K562E did not induce disease-like phenotype. In Mtm1–/y mice, K562E mutant markedly improved muscle force, mass, and fiber size, while others failed to rescue. Therefore, we generated Mtm1–/y Dnm2K562E/+ mice, which showed full rescue of survival, motor function, and muscle force, with improved muscle mass, fiber size, and organelle positioning despite persistently elevated DNM2 levels. This study reveals that DNM2 lipid binding, not protein abundance or GTPase activity, drives pathology, and represents the most rational therapeutic target for DNM2 therapy in MTM1-CNM.
Authors
Raquel Gómez-Oca, Xènia Massana-Muñoz, David Reiss, Juliana De Carvalho Neves, Nadege Diedhiou, Roberto Silva-Rojas, Belinda S. Cowling, Marie Goret, Jocelyn Laporte
Abstract
T cells are the central players in antitumor immunity, and effective tumor killing depends on their ability to infiltrate into the tumor microenvironment (TME) while maintaining normal cytotoxicity. However, late-stage tumors develop immunosuppressive mechanisms that impede T cell movement and induce exhaustion. Investigating T cell migration in human tumors in vivo could provide insights into tumor immune escape, although it remains a challenging task. In this study, we developed ReMiTT, a computational method that leverages spatial transcriptomics data to track T cell migration patterns within tumor tissue. Applying ReMiTT to multiple tumor samples, we identified potential migration trails. On these trails, chemokines that promote T cell trafficking displayed an increasing trend. Additionally, we identified key genes and pathways enriched on these migration trails, including those involved in cytoskeleton rearrangement, leukocyte chemotaxis, cell adhesion, leukocyte migration, and extracellular matrix remodeling. Furthermore, we characterized the phenotypes of T cells along these trails, showing that the migrating T cells are highly proliferative. Our findings introduce an approach for studying T cell migration and interactions within the TME, offering valuable insights into tumor-immune dynamics.
Authors
Lin Zhong, Bo Li, Zhikai Chi, Siyuan Zhang, Qiwei Li, Guanghua Xiao
Abstract
Metabolic adaptation to both caloric excess and restriction promotes energy conservation by suppressing catabolic pathways via feedback mechanisms that remain incompletely defined. We identified TANK binding kinase 1 (TBK1) as a nutrient- and inflammation-responsive brake on AMPK signaling in adipocytes. Fasting or pharmacological AMPK activation induced Tbk1 transcription via a PGC1α/nuclear respiratory factor 1 axis, which, in turn, limited AMPK activity through a phosphorylation cascade to conserve energy. In obesity, this AMPK/TBK1 axis was disrupted due to chronically elevated basal TBK1, thereby restricting energy expenditure during fasting. Adipocyte-specific TBK1 deletion enhanced fasting-induced AMPK activation, mitochondrial function, and lipolytic gene expression in both lean and obese mice. Pharmacological TBK1 inhibition with amlexanox recapitulated these effects. Combined treatment of mice with amlexanox and the AMPK activator AICAR enhanced weight loss, improved glucose tolerance and insulin sensitivity, and suppressed inflammatory and lipogenic programs in adipose tissue, as well as fibrotic gene expression in the liver. Building on prior clinical observations linking TBK1 inhibition to metabolic health, these findings defined a nutrient-sensitive AMPK/TBK1 feedback loop that limited adipocyte catabolism and suggested that dual targeting of TBK1 and AMPK may help counteract metabolic adaptation and enhance the durability of obesity therapies.
Authors
Churaibhon Wisessaowapak, Yuliya Skorobogatko, Hyeonhui Kim, Xue Feng, Seunghwan Son, Haipeng Fu, Sitao Zhang, Pichaya Lertvilai, Lina Chang, Annie Hoang, Hetty Chen, Sarah Bedsted, Joseph Valentine, Jin Young Huh, Peng Zhao, Shannon M. Reilly, Piyajit Watcharasit, Maryam Ahmadian, Alan R. Saltiel
Abstract
Human islet antigen reactive CD4+ memory T cells (IAR T cells) play a key role in the pathogenesis of autoimmune type 1 diabetes (T1D). Using single-cell RNA sequencing (scRNA-Seq) to identify T cell receptors (TCRs) in IAR T cells, we have identified a class of TCRs that share TCRα chains between individuals (“public” chains). We isolated IAR T cells from blood of healthy, new-onset T1D and established T1D donors using multiplexed CD154 enrichment and identified paired TCRα/β sequences from 2767 individual cells. More than a quarter of cells shared TCR junctions between 2 or more cells (“expanded”), and 29/47 (~62%) of expanded TCRs tested showed specificity for islet antigen epitopes. Public TCRs sharing TCRα junctions were most prominent in new-onset T1D. Public TCR sequences were more germline like than expanded unique, or “private,” TCRs, and had shorter junction sequences, suggestive of fewer random nucleotide insertions. Public TCRα junctions were often paired with mismatched TCRβ junctions in TCRs; remarkably, a subset of these TCRs exhibited cross-reactivity toward distinct islet antigen peptides. Our findings demonstrate a prevalent population of IAR T cells with diverse specificities determined by TCRs with restricted TCRα junctions and germline-constrained antigen recognition properties. Since these “innate-like” TCRs differ from previously described immunodominant TCRβ chains in autoimmunity, they have implications for fundamental studies of disease mechanisms. Self-reactive restricted TCRα chains and their associated epitopes should be considered in fundamental and translational investigations of TCRs in T1D.
Authors
Peter S. Linsley, Fariba Barahmand-pour-Whitman, Elisa Balmas, Hannah A. DeBerg, Kaitlin J. Flynn, Alex K. Hu, Mario G. Rosasco, Janice Chen, Colin O’Rourke, Elisavet Serti, Vivian H. Gersuk, Keshav Motwani, Howard R. Seay, Todd M. Brusko, William W. Kwok, Cate Speake, Carla J. Greenbaum, Gerald T. Nepom, Karen Cerosaletti
Abstract
Metabolic dysfunction–associated steatotic liver disease (MASLD) is a global health concern with limited interventions. While the role of gut bacteria in MASLD has been extensively studied, the contribution of gut fungi remains largely unexplored. This study investigates the impact of fungal dysbiosis and the role of CARD9, a key adaptor protein in fungal sensing on gut-liver axis dysfunction in MASLD. Patients with advanced liver fibrosis exhibited distinct mycobiota profiles. Using a Card9-deficient mouse model subjected to high-fat, high-glucose/-fructose feeding, we observed exacerbated liver injury and fibrosis accompanied by fungal dysbiosis, paralleling our findings in human patients. Beyond its established expression in myeloid cells, CARD9 was also detected in intestinal enterocytes where its expression was diminished under metabolic stress. Intestinal organoids with CARD9 inhibition had reduced expression of antimicrobial Reg3g, the tight junction protein ZO-1, and the antifungal enteroendocrine hormone PYY. These findings suggest that CARD9 maintains gut barrier integrity, preventing microbial translocation and subsequent liver injury and fibrosis. Our results provide insights into the interplay between fungal dysbiosis, gut barrier dysfunction, and MASLD, and identify CARD9 as a key protein within this axis.
Authors
Vijay Pandyarajan, So Yeon Kim, Takashi Tsuchiya, Selena Liu, Sadam H. Bhat, Jieun Kim, David M. Underhill, Mazen Noureddin, Shelly C. Lu, Ekihiro Seki
Abstract
Patients with COVID-19 who develop platelet-activating antibodies represent a subset at heightened thrombotic risk, yet the immune features associated with this response remains to be defined. We applied single-cell RNA-seq of B and T cells, single B cell V(D)J-seq, and plasma cytokine and chemokine analysis to define immune signatures distinguishing patients who did (PEA+) or did not (PEA–) develop these antibodies. Patients positive for PEA showed prominent transcriptional enrichment of inflammatory, antigen presentation, and B cell receptor signaling pathways within antigen-experienced B cell subsets. Expanded B cell clones in patients positive for PEA were disproportionately enriched within atypical memory B cells and exhibited upregulated IFN-γ–response signatures, increased proliferative mutational patterns, limited class switching, and a significant overrepresentation of RKH/Y5 heavy-chain motifs associated with platelet-activating antibodies, consistent with an extrafollicular-biased response. Parallel T cell profiling revealed IL-12 pathway enrichment across most T cell subsets, increased IFN-γ transcription, and elevated plasma levels of Th1-associated cytokines in patients positive for PEA. Collectively, these data highlight a coordinated inflammatory environment marked by Th1-skewed T cell activation and selective expansion of atypical memory B cell clones carrying RKH/Y5 motifs, defining immunologic features associated with platelet-activating antibody development in COVID-19.
Authors
Nathan Witman, Mei Yu, Yuqi Zhang, Kexin Gai, Yuhong Chen, Lu Zhou, Christine Nguyen, Wen Zhu, Yongwei Zheng, Shawn Jobe, Mary Beth Graham, Weiguo Cui, Demin Wang, Renren Wen
Abstract
Dengue virus (DENV) vaccines should be designed to induce balanced protective immunity to all 4 DENV serotypes to mitigate the risk of vaccine-enhanced dengue disease. The first tetravalent live DENV vaccine (Dengvaxia) tested in humans was efficacious in children who were partially immune to DENV at baseline. In DENV-naive children, the vaccine was not efficacious and placed some children at risk of more severe WT DENV breakthrough infections. To define dengue vaccine responses at the individual patient level and their relationship to mild and severe dengue infections, we prospectively studied a cohort of DENV-naive children who received 1 dose of Dengvaxia. The vaccine stimulated variable responses that neutralized 0, 1 (monotypic), or 2+ (multitypic) serotypes in individual children. Using a logistic regression model, we found that vaccinated children with neutralizing antibody (NAb) to 1 serotype only were at greater risk developing dengue compared with children who were not vaccinated (odds ratio 5.07). This risk was not observed in vaccinated children with no NAb or NAb to 2 or more serotypes. We propose that individuals with durable NAb to 1 serotype have an abundance of serotype cross-reactive, nonneutralizing antibodies implicated in the enhanced replication of heterologous serotypes.
Authors
Laura J. White, Lindsay D. Hein, Maria Abad Fernandez, Cameron Adams, Elizabeth Adams, Emily Freeman, Ruby Shah, Lakshmanane Premkumar, Kristal An Agrupis, Maria Vinna Crisostomo, Jedas Veronica Daag, Michelle Ylade, Jacqueline Deen, Ana Lena Lopez, Leah Katzelnick, Aravinda M. de Silva
Abstract
Insulin and glucagon are described as having opposing actions on hepatic glycogen metabolism. However, here we showed that their coordinated action promoted glycogen turnover and meal glucose storage. In mice, pharmacological doses of insulin or glucagon failed to alter hepatic glycogen, but the combination produced a robust decrease in glycogen content. Additivity between insulin and glucagon was also seen with the activation of hepatic insulin signaling intermediates. This signaling pathway drove glycogen synthesis, suggesting concurrent actions on glycogen breakdown and repletion. A mixed nutrient meal, which stimulates an increase in both insulin and glucagon, enhanced the incorporation of dietary glucose into hepatic glycogen. This was much more pronounced than the effects of glucose alone, which only stimulated insulin secretion. These findings revealed that glucagon is required for efficient hepatic glucose storage when acting in concert with insulin. Coordinated insulin-glucagon signaling, thus, emerged as a critical mechanism for hepatic glycogen cycling, challenging the classical paradigm that these hormones work in opposition.
Authors
Nidhi Kejriwal, David Bouslov, Cheyenne R. Castle, Riya S. Karve, Galina A. Arkharova, Ashot Sargsyan, Daniel J. Drucker, Guo-Fang Zhang, David A. D’Alessio, Jonathan E. Campbell, Megan E. Capozzi
No posts were found with this tag.