Immunology
Abstract
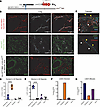
Lung IL-33 is involved in pathogen defense, barrier homeostasis, and development of allergic responses. We previously identified a 5 kb noncoding region within a GWAS-defined segment that regulates expression of human IL33 (hIL33) but is absent in the murine locus. To understand how this region affects IL-33 expression in vivo, we engineered 2 BAC-transgenic strains in which 166 kb of the human genome upstream of the hIL33 locus, along with a fluorescent reporter, was inserted into the murine genome, both with and without the 5 kb region. Comparison to a murine Il33 (mIl33) reporter strain revealed species-specific tropism; hIL33 reporter was mostly expressed in the endothelium, while mIl33 reporter was expressed in type 2 alveolar epithelium. hIL33 reporter expression in tracheal basal epithelium, submucosal glands, and lung microvasculature required the 5 kb region. Surprisingly, allergen and exogenous IL-33 downregulated hIL33 reporter in lung endothelium only when the 5 kb region was present. Similar IL-33–dependent downregulation of IL33 transcripts was observed in human endothelial cell lines, validating that our hIL33 reporter strain recapitulated human endothelial biology. Together, these data reveal the importance of the asthma-associated human 5 kb region in regulating human IL33 expression in a cell type– and context-dependent manner.
Authors
Maile K. Hollinger, Chanie L. Howard, Donna C. Decker, Kelly M. Blaine, Ivy Aneas, Emily M. Grayson, Tania E. Velez, Fernando A. Oliveira, Riley T. Hannan, Daniel F. Camacho, Philip A. Verhoef, Cara L. Hrusch, Rebecca S. Griffes, Jeffrey M. Sturek, Marcelo A. Nobrega, Nathan Schoettler, Anne I. Sperling
Abstract
T cells are the central players in antitumor immunity, and effective tumor killing depends on their ability to infiltrate into the tumor microenvironment (TME) while maintaining normal cytotoxicity. However, late-stage tumors develop immunosuppressive mechanisms that impede T cell movement and induce exhaustion. Investigating T cell migration in human tumors in vivo could provide insights into tumor immune escape, although it remains a challenging task. In this study, we developed ReMiTT, a computational method that leverages spatial transcriptomics data to track T cell migration patterns within tumor tissue. Applying ReMiTT to multiple tumor samples, we identified potential migration trails. On these trails, chemokines that promote T cell trafficking displayed an increasing trend. Additionally, we identified key genes and pathways enriched on these migration trails, including those involved in cytoskeleton rearrangement, leukocyte chemotaxis, cell adhesion, leukocyte migration, and extracellular matrix remodeling. Furthermore, we characterized the phenotypes of T cells along these trails, showing that the migrating T cells are highly proliferative. Our findings introduce an approach for studying T cell migration and interactions within the TME, offering valuable insights into tumor-immune dynamics.
Authors
Lin Zhong, Bo Li, Zhikai Chi, Siyuan Zhang, Qiwei Li, Guanghua Xiao
Abstract
TB (Tuberculosis) and HIV co-infection remains a major global health challenge, with limited understanding of how these pathogens impact local immune responses in the lungs. This study is the first to investigate the modulation of IL-21 during LTBI and Mycobacterium tuberculosis (Mtb)/ Simian Immunodeficiency Virus (SIV) co-infection in non-human primates (NHP). We show that IL-21 expression, predominantly derived from CD4⁺ T cells, is significantly reduced in lungs of Mtb/SIV co-infected macaques, especially in the absence of cART. Although cART and cART with 3HP partially restore IL-21-producing CD4⁺ T cells, levels remain below those in LTBI, indicating ongoing immune impairment. Spatial transcriptomic analysis suggests localized alterations in immune signaling, including differences in STAT1- and STAT3-associated transcriptional profiles and reduced Mtb-specific IFN-γ responses in co-infected animals. Together, our findings indicate that IL-21-producing CD4⁺ T cells are selectively and persistently impaired in the lungs during Mtb/SIV co-infection despite antimicrobial and antiviral therapy. These results highlight a compartment-specific deficit in immune reconstitution and suggest that IL-21-associated pathways may warrant further investigation as potential targets for host-directed therapeutic strategies.
Authors
Vinay Shivanna, Renee D. Escalona, Colin Chuba, Shashi Prakash Singh, Ahmed A. Moustafa, J. Quincy Brown, Chenyao Xiao, Sangkyu Kim, Edward J. Dick Jr., Smriti Mehra, Mirko Paiardini, Riti Sharan
Abstract
BACKGROUND. Chimeric antigen receptor T-cell (CAR-T) therapies have revolutionized treatment for relapsed/refractory multiple myeloma (RRMM). However, cytokine release syndrome (CRS), a common and potentially severe complication, requires inpatient monitoring, limiting access and increasing costs. Wearable devices could support outpatient CAR-T delivery, but feasibility for CRS detection versus standard care remains unproven. METHOD. We conducted a prospective, single-center observational pilot study to assess the feasibility of using wearable devices for monitoring vital signs and detecting CRS. Thirty patients receiving idecabtagene vicleucel (ide-cel) or ciltacabtagene autoleucel (cilta-cel) were enrolled; 25 with sufficient monitoring data were evaluable. Sensors collected skin and axillary temperature, oxygen saturation, respiratory and heart rate, and motion. Peripheral blood cytokines were analyzed pre- and post-infusion using a multiplex proteomic platform. The primary outcome was feasibility, assessed by CRS detection sensitivity and specificity; secondary outcomes included adherence, lead time, and performance of models integrating wearable and cytokine data. RESULTS. CRS occurred in 20 of 25 patients. The best-performing wearable model detected 18 or 20 CRS episodes with a sensitivity of 0.72 (mean 0.75; 95% CI 0.60–0.91) and a specificity of 0.80 (mean 0.76; 95% CI 0.68–0.84), and a median lead time of 7:00 hours before nursing recognition. Median adherence during high-risk periods was 71%. Cytokine changes paralleled temperature elevations, and IFN-γ emerged as a consistent biomarker. CONCLUSION. Wearable devices are feasible for early CRS detection and may support outpatient CAR-T care. Larger outpatient studies are warranted. TRIAL REGISTRATION. This study did not meet the criteria for ClinicalTrials.gov registration.
Authors
Sridevi Rajeeve, Matt Wilkes, Nicole Zahradka, Lewis Tomalin, Mujahid Quidwai, Darren Pan, Nicholas J. Calafat, Martin Cusack, Adolfo Aleman, Kseniya Serebryakova, Katerina Kappes, Hayley Jackson, Sarita Agte, Santiago Thibaud, Larysa Sanchez, Shambavi Richard, Joshua Richter, Cesar Rodriguez, Hearn Jay Cho, Ajai Chari, Sundar Jagannath, Alessandro Laganà, Adriana C. Rossi, Samir Parekh
Abstract
Immune checkpoint inhibitors have transformed cancer therapy, yet many patients fail to achieve durable responses due to insufficient T cell reinvigoration. Cytokines offer promise for enhancing immunotherapy, but their clinical use is limited by toxicity and a narrow therapeutic index. Immunocytokines, engineered fusion proteins combining antibody specificity with cytokine activity, aim to overcome these challenges by targeting cytokine delivery to immune cells or the tumor microenvironment. We describe SAR445877 (SAR’877), a novel PD-1-targeted immunocytokine that fuses a high-affinity anti-PD-1 antibody with a detuned IL-15/IL-15Rα sushi domain complex. SAR’877 blocks PD-1/PD-L1 and PD-1/PD-L2 interactions while selectively delivering IL-15 signals to PD-1+ T cells, enhancing proliferation and activation of antigen-experienced CD8+ and CD4+ T cells and NK cells, while minimizing systemic inflammation. Mechanistically, SAR’877 activates STAT5 signaling in PD-1+ lymphocytes and restores effector function in exhausted T cells. In preclinical models, a murine surrogate of SAR’877 accelerated viral clearance and induced robust anti-tumor immunity by expanding cytotoxic CD8+ T cells and promoting Th1 polarization. Notably, SAR’877 outperformed anti-PD-1 plus untargeted IL-15, highlighting the therapeutic potential of targeted IL-15 delivery. These findings position SAR’877 as a promising next-generation immunotherapy with enhanced efficacy and reduced cytokine-associated toxicities.
Authors
Isaraphorn Pratumchai, Marie Bernardo, Julien Tessier, Jaroslav Zak, Kristi L. Marquardt, Joon Sang Lee, Maheeka Bimal, AHyun Choi, Anthony M. Byers, Mikielia G. Devonish, Roberto Carrio, Dan Lu, Stella A. Martomo, Jeegar Patel, Yu-an Zhang, Ingeborg M. Langohr, Virna Cortez-Retamozo, Dinesh S. Bangari, Angela Hadjipanayis, Xiangming Li, Valeria R. Fantin, Donald R. Shaffer, John R. Teijaro
Abstract
Tumor-infiltrating CD8 cells recognize neoantigens created by tumor-specific mutations. Nonetheless, even after checkpoint inhibitor therapy, most patients progress. A deeper understanding of anti-tumor responses could facilitate development of better therapies. To enable such studies, we applied TCXpress, a high throughput platform that clones fully expressible TCRs from single cells into retro- or lenti- viral vectors without sequencing or gene synthesis, to study TCRs from CD8 cells infiltrating mouse MC38 tumors. We expressed cloned TCRs in reporter cells and interrogated TCR specificity by coculturing them with B6WT3 cells transduced with tandem minigenes encoding predicted neoantigens. We isolated TCRs reactive against epitopes from mutant Rpl18, Adpgk, Psmd2, and Zc3h7b along with self-reactive TCRs that recognized normal B6 and MC38 cells. Importantly, we successfully treated MC38-bearing mice with T cells transduced with anti-Rpl18 TCRs. These results establish a system that could be used to study many types of T cell responses and validates a therapeutic approach that could be tested in the clinic.
Authors
Alexander M. Rowe, Smriti Chaurasia, Wenzhong Wei, Laura García-Diéguez, Katherine Querry, Johnathon G. Schiebel, Christy Smolak, Alexander G. Muralles, Daniel Wikenheiser, Kevin Quann, Collin Pirner, Kentin Codispot, Mark J. Shlomchik, Warren D. Shlomchik
Abstract
Enhancing NAD+ levels with nicotinamide riboside (NR) confers anti-inflammatory effects in human disease, although immunoregulatory mechanisms remain poorly characterized. We previously showed that ex vivo NR supplementation of primary CD4+ T cells from psoriatic individuals dampened immune responsiveness. To validate this in vivo, we performed a randomized, placebo-controlled NR supplementation study in individuals with mild-to-moderate psoriasis. Participants received oral NR (500 mg twice daily) or matching placebo for 4 weeks, with blood samples collected at baseline and after supplementation. NR reduced Th17 immune responsiveness. Bulk CD4+ T cell RNA-seq identified induction of the SLIT-ROBO signaling pathway. NR supplementation increased circulating SLIT2 levels and enhanced SLIT2 production in dermal fibroblasts. Pharmacologic and genetic interrogation in CD4+ T cells and fibroblasts demonstrated that SLIT2, acting through the ROBO1 receptor, inhibited Rho GTPase signaling, thereby attenuating canonical Th17 polarization and fibroblast inflammatory activation. These findings indicate that NAD+ augmentation exerts anti-inflammatory effects in psoriasis through SLIT2-ROBO1-mediated crosstalk between dermal fibroblasts and circulating CD4+ T cells, leading to suppression of Th17-driven inflammation.
Authors
Kim Han, Rachael J. Klein, Thomas C. Recupero, Anna Chiara Russo, Rahul Sharma, Anand K. Gupta, Shahin Hassanzadeh, Rebecca D. Huffstutler, Pradeep K. Dagur, Bryan Fisk, Neelam R. Redekar, Michael N. Sack
Abstract
CHI3L1, a chitinase-like protein, is implicated in pulmonary fibrosis, yet its mechanisms incompletely understood. In this study, we demonstrated that CHI3L1 coordinates profibrotic macrophage activation and invasive myofibroblast differentiation, and their crosstalk. In vitro, CHI3L1 drove M2-like macrophage polarization as evidenced by increased CD163, CD206, and PD-L1, and amplified TGF-β1-induced fibroblast responses, including myofibroblast transformation, migration, and invasion. Mechanistically, CHI3L1 enhanced TGF-β1 signaling through SMAD, AKT, and ERK pathways, and PD-L1 was required for CHI3L1/TGF-β1-driven myofibroblast transformation. Co-culture studies further demonstrated the ability of CHI3L1 to induce profibrotic macrophage activation that enhanced myofibroblast transformation mediated via a CD44–PD-L1 axis. In vivo, following bleomycin challenge, CHI3L1 transgenic mice exhibited increased PD-L1+ M2 macrophages, PD-L1+/PDGFRα+ fibroblasts, and PD-1+ immune cells compared with wild-type controls. Therapeutically, combined anti-CHI3L1 and anti-PD-1 antibodies, as well as a bispecific anti-CHI3L1-anti-PD-1 antibody, produced greater anti-fibrotic efficacy than monotherapy. These findings demonstrate crosstalk between CHI3L1 and the PD-1/PD-L1 pathway that promotes profibrotic macrophage activation and invasive fibroblast differentiation and support dual targeting of CHI3L1 and PD-1/PD-L1 as a promising therapeutic strategy for pulmonary fibrosis.
Authors
Han-Seok Jeong, Takayuki Sadanaga, Joyce H. Lee, Suchitra Kamle, Bing Ma, Yang Zhou, Sung Jae Shin, Jack A. Elias, Chun Geun Lee
Abstract
Eosinophilic esophagitis (EoE) is a type 2 allergic disease characterized by esophageal inflammation and epithelial cell dysfunction. The acquired loss of the anti-serine protease of kazal type 7 (SPINK7) in the squamous epithelium of the esophagus has a causal role in EoE pathogenesis. Yet there is a limited understanding of the factors that regulate its expression and responsiveness to inflammatory stimuli. Herein, we have identified the transcription factor, ovo like transcriptional repressor 1 (OVOL1) as an esophageal selective gene product that regulates SPINK7 promoter activity. Overexpression of OVOL1 increased SPINK7 expression, whereas its depletion decreased SPINK7 expression, impaired epithelial barrier and increased production of the pro-atopy cytokine thymic stromal lymphopoietin (TSLP). Stimulation with IL-13 abrogated the nuclear translocation of OVOL1 and promoted enhanced degradation of OVOL1 protein. This effect of IL-13 was dependent on the esophageal specific cysteine protease calpain-14 at least in part. Analysis of human esophageal biopsies demonstrated that the expression of esophageal OVOL1 correlated with SPINK7 transcript expression and was lost as a function of EoE disease activity. In summary, our study identifies key regulatory mechanisms in EoE pathogenesis, demonstrating that OVOL1 promotes SPINK7 transcription, whereas IL-13 suppresses this pathway in EoE.
Authors
Nurit P. Azouz, Andrea M. Klingler, Sierra S. Beach, Kalen A. Rossey, Mark Rochman, Misu Paul, Julie M. Caldwell, Michael Brusilovsky, Alexander T. Dwyer, Xiaoting Chen, Daniel Miller, Carmy Forney, Leah C. Kottyan, Matthew T. Weirauch, Marc E. Rothenberg
Abstract
Human γδ T cells are a rare but functionally diverse lymphocyte subset critical for tumor surveillance and antimicrobial immunity. Although they express natural killer (NK) cell-associated receptors such as Killer-cell Immunoglobulin-like Receptors (KIRs), the relevance of KIR expression on γδ T cells remains largely unexplored. Using flow cytometry, ATAC-seq and RNA-seq, we identified KIR expression as a marker that distinguished two functionally and molecularly distinct γδ T cell subsets. KIR⁺ γδ T cells exhibited an advanced, memory-like differentiation state characterized by heightened cytotoxicity, stable epigenetic remodeling and a predominant IFNγ-producing profile. In contrast, KIR⁻ γδ T cells maintained a naïve-like phenotype and preferentially produced IL-17 upon polarization. Notably, KIR+ γδ T cells were consistently observed across individuals but were significantly enriched in cytomegalovirus (CMV)-seropositive donors, suggesting that chronic antigenic stimulation could promote the emergence of KIR⁺ effector γδ T cells. These findings reveal a functional dichotomy in human γδ T cells defined by KIR expression, linking IFNγ-driven cytotoxicity with KIR⁺ cells and IL-17 production with KIR⁻ cells. This insight advances our understanding of γδ T cell heterogeneity and has implications for viral immunity, immune memory and the development of γδ T cell-based immunotherapies.
Authors
Mahya Razmi, Yeganeh Almasi, Marilee Larrivée, Jonathan B. Angel, Alexandre Blais, Zakia Djaoud
No posts were found with this tag.