Endocrinology
Abstract
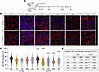
HNF1A-MODY, the most common monogenic diabetes, exhibits progressive β cell dysfunction, but existing mouse models fail to recapitulate human disease progression, limiting understanding of pathogenic mechanisms. We developed mice with heterozygous deletion of the Hnf1a transactivation domain (Hnf1a+/Δe4-10) to model human HNF1A haploinsufficiency, conducted cross-sectional metabolic characterization, and validated our findings in HNF1A-deficient human islets. Unlike previous models, Hnf1a+/Δe4-10 mice successfully recapitulated temporal HNF1A-MODY progression. Male mice developed sequential pathophysiology: early insulin resistance in young adults (7 weeks), followed by testosterone deficiency and fasting hyperglycemia in adult mice (10 weeks). Glucose intolerance emerged in middle-aged mice (30 weeks), progressing to multi-organ dysfunction in aged mice (44–70 weeks), characterized by elevated hepatic gluconeogenesis, impaired renal glucose handling, and hepatic steatosis/fibrosis. This dual pathophysiology involving β cell dysfunction and peripheral insulin resistance was associated with dysregulated hormone secretion from both α and β cells in aged mice (40–70 weeks). Human islet studies with HNF1A knockdown confirmed translational relevance, demonstrating reduced SGLT2 protein expression and inappropriate glucagon and insulin secretion. This work established a physiologically relevant HNF1A-MODY model, identified early insulin resistance as a key mechanism triggering hormonal dysfunction, and revealed HNF1A’s role in multi-organ pathophysiology beyond traditional β cell dysfunction.
Authors
Isaline Louvet, Ana Acosta-Montalvo, Chiara Saponaro, Maria Moreno-Lopez, Sana Douffi, Abdelkrim El Karchaoui, Gianni Pasquetti, Julien Thevenet, Nathalie Delalleau, Valery Gmyr, Paolo Giacobini, Stéphanie Espiard, Julie Kerr-Conte, François Pattou, Adrian Liston, Caroline Bonner
Abstract
Metabolic adaptation to both caloric excess and restriction promotes energy conservation by suppressing catabolic pathways via feedback mechanisms that remain incompletely defined. We identified TANK binding kinase 1 (TBK1) as a nutrient- and inflammation-responsive brake on AMPK signaling in adipocytes. Fasting or pharmacological AMPK activation induced Tbk1 transcription via a PGC1α/nuclear respiratory factor 1 axis, which, in turn, limited AMPK activity through a phosphorylation cascade to conserve energy. In obesity, this AMPK/TBK1 axis was disrupted due to chronically elevated basal TBK1, thereby restricting energy expenditure during fasting. Adipocyte-specific TBK1 deletion enhanced fasting-induced AMPK activation, mitochondrial function, and lipolytic gene expression in both lean and obese mice. Pharmacological TBK1 inhibition with amlexanox recapitulated these effects. Combined treatment of mice with amlexanox and the AMPK activator AICAR enhanced weight loss, improved glucose tolerance and insulin sensitivity, and suppressed inflammatory and lipogenic programs in adipose tissue, as well as fibrotic gene expression in the liver. Building on prior clinical observations linking TBK1 inhibition to metabolic health, these findings defined a nutrient-sensitive AMPK/TBK1 feedback loop that limited adipocyte catabolism and suggested that dual targeting of TBK1 and AMPK may help counteract metabolic adaptation and enhance the durability of obesity therapies.
Authors
Churaibhon Wisessaowapak, Yuliya Skorobogatko, Hyeonhui Kim, Xue Feng, Seunghwan Son, Haipeng Fu, Sitao Zhang, Pichaya Lertvilai, Lina Chang, Annie Hoang, Hetty Chen, Sarah Bedsted, Joseph Valentine, Jin Young Huh, Peng Zhao, Shannon M. Reilly, Piyajit Watcharasit, Maryam Ahmadian, Alan R. Saltiel
Abstract
Chronic hyperglycemia induces microvascular complications in patients with type 2 diabetes (T2D), particularly diabetic retinopathy, nephropathy, and neuropathy. We revisited to examine such vascular damage in the pancreas in 3D. Using thick pancreatic tissue slices, we analyzed volumetric intraislet and peri-islet exocrine capillary density (vICD and vECD), as well as interface capillary counts along the islet periphery to quantify vascular integration between the islets and surrounding acinar cells. Contrary to the previous reports, vICD was not homogeneous, but highly heterogeneous across the five species studied (human, monkey, pig, ferret and mouse), especially in smaller islets (15%–80%). vICD became less variable with increasing islet size converging at approximately 20%. With this foundation of islet vascularization, pancreatic tissues from non-diabetic (ND) and T2D subjects consisting of eight age- and sex-matched pairs (age range of 35-65 years with various duration: 0-15 years) were examined. Strikingly, no significant differences in microvasculature were found, where mean vICD (~30%) and mean vECD (~15%) were nearly equivalent between the groups. Capillary integration with respect to islet size was comparable. It suggests that integrated pancreatic blood flow with robust crosstalk between the endocrine and exocrine pancreas may facilitate microvascular preservation in T2D via local distribution of insulin.
Authors
Alex M. Tollefson, Frank R. Marsico, Manami Hara
Abstract
Hypothalamic melanocortin 4 receptors (MC4Rs) play a central role in regulating food intake and energy homeostasis. In fact, inactivating mutations in the MC4R gene are the most common form of monogenic obesity. Agonist activation of MC4Rs reduces food intake by modulating hypothalamic signaling circuits. Thus, a detailed understanding of the signaling pathways that regulate MC4R activity is of considerable translational relevance. Ligand-activated MC4Rs interact not only with heterotrimeric G proteins but can also recruit beta-arrestin-2 (barr2) to the receptor. The potential functional role of barr2 in regulating the anorectic effects of MC4R signaling remains unexplored. In the present study, we used mutant mouse models to demonstrate that MC4R-mediated activation of barr2/ERK signaling in MC4R neurons of the paraventricular nucleus leads to reduced food intake. We also found that the appetite-suppressing effect of setmelanotide, an MC4R agonist approved by the FDA for the treatment of certain types of obesity, requires the presence of barr2 in MC4R-containing neurons. These data suggest that MC4R agonists able to promote MC4R/barr2 interactions with high efficacy may become useful as appetite-suppressing drugs.
Authors
Misbah Rashid, Lei Wang, Zhenzhong Cui, Oksana Gavrilova, Huiyan Lu, Kozo Kaibuchi, Sarah Zeitlmayr, Thomas Gudermann, Andreas Breit, Jürgen Wess
Abstract
Authors
Anna J. Son, Emmanuel Rapp, Alex Wiezorek, Max G. Leung, Ronadip R. Banerjee, Thomas H. Leung
Abstract
Thyroid hormone signaling is an essential regulator of skeletal muscle development, function, and metabolism, yet the specific signaling pathways required for muscle regeneration are not yet defined. We used scRNA-seq and the FUCCI (fluorescent ubiquitination-based cell cycle indicator) reporter mouse model to examine how hypothyroidism impacts repair processes after cardiotoxin-induced injury in mice. During regeneration, and up to 2 months after injury, hypothyroid muscles displayed smaller myofibers and a shift to slower oxidative fiber types. scRNA-seq of tibialis anterior muscle during regeneration revealed that hypothyroidism reduced myogenic-lineage diversity. Cell cycle analysis confirmed delayed cell cycle progression at 5 and 14 days after injury, with skeletal muscle stem cells stalled at the G1/S transition, hindering differentiation. Transcriptomic data revealed altered nonmyogenic dynamics, including elevated activated fibro-adipogenic progenitors (FAPs) early in repair and persistent proinflammatory macrophages. Integrative regulon and ligand-receptor analysis further demonstrated that triiodothyronine acted through dual modes: a direct transcriptional control of myogenic cell cycle and oxidative programs and an indirect paracrine remodeling mediated by FAP and immune signaling networks. This study identified what we believe to be novel effects of hypothyroidism on myogenic heterogeneity and impaired tissue repair, offering insights into muscle-wasting mechanisms relevant to hypothyroidism-associated myopathy and sarcopenia.
Authors
Paola Aguiari, Valentina Villani, Yan-Yun Liu, Gianni Carraro, Gregory A. Brent, Laura Perin, Anna Milanesi
Proteomic analyses of human islets reveal potential markers of β-cell dysfunction during prediabetes
Abstract
The mechanisms driving progressive beta-cell dysfunction in type 2 diabetes (T2D) remain incompletely understood. This study aimed to identify pancreatic islet proteome changes that could predict diabetes onset. We isolated islets from non-diabetic subjects undergoing partial pancreatectomy, previously characterized for glucose tolerance, insulin sensitivity, and insulin secretion, using laser capture microdissection (LCM) and analyzed them via high-performance liquid chromatography-mass spectrometry (HPLC-MS). Proteomic analysis revealed that subjects with impaired glucose tolerance (IGT) had reductions in proteins regulating glycolysis (PGK1, G3P), lipid metabolism (ACBP, ARF1), glucose transport (14-3-3B), and insulin secretion (STARD10, CAPDS) compared to normal glucose tolerant (NGT) subjects. Additionally, IGT islets showed impaired expression of proteins involved in glucose- and incretin-stimulated insulin response (CREB1, IQGA1). Stratification by beta-cell glucose sensitivity (βGS) indicated that subjects with lower βGS exhibited reduced levels of insulin maturation (ERO1B) and anti-apoptotic proteins (CASP8, PAK2, SKP1), along with increased SEL1L, a factor promoting endocrine precursor differentiation. These findings suggest that early defects in glucose metabolism and insulin secretion characterize IGT, while reduced βGS may trigger compensatory mechanisms, through enhanced beta-cell survival or neogenesis, to delay T2D progression. Overall, proteomic alterations in prediabetic islets provide potential early predictive markers and targets for interventions aimed at preserving beta-cell function.
Authors
Chiara Maria Assunta Cefalo, Teresa Mezza, Giuseppe Quero, Sergio Alfieri, Donatella Lucchetti, Filomena Colella, Alessandro Sgambato, Wei-Jun Qian, Andrea Mari, Alfredo Pontecorvi, Andrea Giaccari, Rohit N. Kulkarni
Abstract
Adipocytes exist along a functional spectrum: white adipocytes are energy storing while brown adipocytes have thermogenic capacity such that activation may counteract obesity-related disease. In between are UCP1-expressing beige adipocytes, which can transition between these two energetic states. We previously showed that bone morphogenetic protein 7 (BMP7), a member of the transforming growth factor-β (TGFβ) superfamily, enables differentiation of brown preadipocytes to mature thermogenic cells. To see if immortalized, clonal human white and brown preadipocytes (hWA and hBA, respectively) would become more thermogenic in response to BMP exposure, we treated them with BMP7 or BMP4 for the first 7d of a 30d differentiation protocol. In hBA, absence of either BMP7 or BMP4 led to lower expression of brown-specific markers and oxygen consumption relative to 7d with either BMP. hWA treated for 7d with either BMP did not increase expression of thermogenic protein UCP1 nor induce a brown-like transcription profile. However, BMP-treated hWA produced adipocytes that had higher basal and drug-induced maximal oxygen consumption, which was UCP1-independent and due substantially to the futile creatine cycle (FCC). Our results demonstrate that energetically quiescent human white preadipocytes can be pushed into an energy expending phenotype without transdifferentiation into beige adipocytes, providing a new approach to treat obesity-related metabolic disease.
Authors
Kelly T. Long, Cheryl Cero, Sahara L. Ali, Nhuquynh Nguyen, Adrienne R. Guarnieri, Ju Hee Kim, Young Jae Bahn, Jurgen Heymann, Jonathan M. Dreyfuss, Sushil G. Rane, Yu-Hua Tseng, Aaron M. Cypess
Abstract
GLP-1 receptor (GLP-1R) agonists decrease blood glucose and body weight and reduce rates of cardiovascular and renal disease. Although GLP-1R activation lowers blood pressure (BP), the underlying mechanisms remain incompletely understood and have been attributed to weight loss and endothelial cell GLP-1R signaling. Here, we show that GLP-1Rs in vascular smooth muscle cells (VSMCs) are essential for semaglutide-mediated BP reduction in mice. In contrast, GLP-1Rs in Tie2+ endothelial or immune cells are not required for semaglutide to lower BP. The VSMC GLP-1R is dispensable for the effects of semaglutide on food intake, body weight, and blood glucose, but is required for its actions to increase glomerular filtration rate and promote natriuresis. Systemic semaglutide administration resulted in proteomic changes in the renal artery and kidney in pathways related to platelet aggregation, fibrin clot formation, lipid metabolism, and pro-apoptotic signaling that are abolished in mice lacking VSMC GLP-1R expression. Moreover, semaglutide directly induced vasorelaxation in pre-constricted mesenteric arteries ex vivo. Together, these findings identify VSMCs as a key cellular target linking GLP-1R activation to BP regulation, renal electrolyte excretion, and proteomic changes in renal artery and kidney.
Authors
Kyle D. Medak, Jacqueline A. Koehler, Laurie L. Baggio, Maria J. Gonzalez-Rellan, Chi Kin Wong, Xiemin Cao, Vivikta Rao, Sean Kao, Yu Cui, Jiayi Fu, Easton Liaw, M. Golam Kabir, Jie Zhang, Jin Wei, Daniel J. Drucker
Abstract
Insulin and glucagon are described to have opposing actions on hepatic glycogen metabolism. However, here we showed that their coordinated action promoted glycogen turnover and meal glucose storage. In mice, pharmacological doses of insulin or glucagon failed to alter hepatic glycogen, but the combination produced a robust decrease in glycogen content. Additivity between insulin and glucagon was also seen with the activation of hepatic insulin signaling intermediates. This signaling pathway drove glycogen synthesis, suggesting concurrent actions on glycogen breakdown and repletion. A mixed nutrient meal, which stimulates an increase in both insulin and glucagon, enhanced the incorporation of dietary glucose into hepatic glycogen. This was much more pronounced than the effects of glucose alone, which only stimulated insulin secretion. These findings revealed that glucagon is required for efficient hepatic glucose storage when acting in concert with insulin. Coordinated insulin-glucagon signaling thus emerged as a critical mechanism for hepatic glycogen cycling, challenging the classical paradigm that these hormones work in opposition.
Authors
Nidhi Kejriwal, David Bouslov, Cheyenne R. Castle, Riya S. Karve, Galina A. Arkharova, Ashot Sargsyan, Daniel J. Drucker, Guo-Fang Zhang, David A. D'Alessio, Jonathan E. Campbell, Megan E. Capozzi
No posts were found with this tag.