Vascular biology
Abstract
Lung IL-33 is involved in pathogen defense, barrier homeostasis, and development of allergic responses. We previously identified a 5 kb noncoding region within a GWAS-defined segment that regulates expression of human IL33 (hIL33) but is absent in the murine locus. To understand how this region affects IL-33 expression in vivo, we engineered 2 BAC-transgenic strains in which 166 kb of the human genome upstream of the hIL33 locus, along with a fluorescent reporter, was inserted into the murine genome, both with and without the 5 kb region. Comparison to a murine Il33 (mIl33) reporter strain revealed species-specific tropism; hIL33 reporter was mostly expressed in the endothelium, while mIl33 reporter was expressed in type 2 alveolar epithelium. hIL33 reporter expression in tracheal basal epithelium, submucosal glands, and lung microvasculature required the 5 kb region. Surprisingly, allergen and exogenous IL-33 downregulated hIL33 reporter in lung endothelium only when the 5 kb region was present. Similar IL-33–dependent downregulation of IL33 transcripts was observed in human endothelial cell lines, validating that our hIL33 reporter strain recapitulated human endothelial biology. Together, these data reveal the importance of the asthma-associated human 5 kb region in regulating human IL33 expression in a cell type– and context-dependent manner.
Authors
Maile K. Hollinger, Chanie L. Howard, Donna C. Decker, Kelly M. Blaine, Ivy Aneas, Emily M. Grayson, Tania E. Velez, Fernando A. Oliveira, Riley T. Hannan, Daniel F. Camacho, Philip A. Verhoef, Cara L. Hrusch, Rebecca S. Griffes, Jeffrey M. Sturek, Marcelo A. Nobrega, Nathan Schoettler, Anne I. Sperling
Abstract
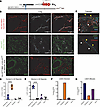
Single-ventricle congenital heart disease (SV-CHD) is a uniformly lethal condition requiring the Glenn surgery, which as a side effect eliminates arterial pulsatility and contributes to pulmonary vascular complications. In Glenn patients, we quantified pulsatility loss in each dimension of force (flow, pressure, and stretch) using cardiac catheterization and MRI. To model and investigate the individual impact of each dimension of pulsatility loss on the pulmonary vasculature, we applied isolated pulsatile and non-pulsatile mechanical stimuli to pulmonary artery endothelial cells (ECs) in vitro. We found that each dimension of force triggered distinct transcriptional responses, revealing force-specific regulation of structural and signaling pathways. Pulsatile stretch uniquely stimulated EC secretion of PDGFB, a key driver of vascular smooth muscle cell (vSMC) recruitment. In a rat Glenn model, loss of pulsatility led to vascular wall thinning, loss of EC PDGFB, and reduced activation of smooth muscle PDGFBRβ, confirming in vivo relevance. Our findings uncover a mechanistic link between endothelial stretch sensing and PDGFB-mediated EC-vSMC crosstalk, essential for maintaining pulmonary artery architecture. Clinically, these insights suggest that restoring or mimicking pulsatile forces may help preserve vascular integrity and prevent remodeling in patients with SV-CHD.
Authors
Stephen B. Spurgin, Lauren Thai, Tina C. Wan, Christopher P. Chaney, Mitzy A. Cowdin, Surendranath Veeram Reddy, Tarique Hussain, Munes Fares, M. Luisa Iruela-Arispe, Thomas Carroll, Andrew D. Spearman, Ondine Cleaver
Abstract
Glaucoma is associated with ocular hypertension, and lowering intraocular pressure is the primary objective of current therapies. Recent studies have established a key role for Schlemm’s canal endothelium in this pressure increase and have shown that it has a unique, lymphatic-like hybrid phenotype characterized by expression of the lymphatic transcription factor PROX1. However, the functional importance of this hybrid phenotype in the adult canal remains unclear, as long-term studies have been limited by systemic requirements for lymphatic gene expression and a lack of Schlemm’s canal–specific animal models. Here, we designed and validated a strategy using 4OH-tamoxifen-loaded nanocarriers to generate targeted, Schlemm’s canal-specific Prox1 knockout mice that specifically lacked lymphatic characteristics in the canal endothelium. Within four weeks, intraocular pressure was significantly elevated, and ocular hypertension was maintained for at least 24 weeks. Unlike lymphatic vessels, which degenerate following Prox1 deletion, Schlemm’s canal persisted but reverted to a less functional vein-like phenotype with no change in size or morphology. Together, these findings demonstrate the utility of nanocarrier-mediated tamoxifen delivery and establish the importance of the Schlemm’s canal lymphatic-like phenotype in intraocular pressure regulation, providing targets for future glaucoma therapies and a mouse model of adult-onset ocular hypertension.
Authors
Sofia Lara Ochoa, Hoi-Lam Li, Hyeohn Kim, Zihang Yan, Natalia C. Mendonca, Pan Liu, Hyunjoo J. Lee, Michael P. Vincent, Sultan Almunif, Hao F. Zhang, Haiyan Gong, Evan A. Scott, Mark Johnson, Benjamin R. Thomson
Abstract
In metabolic dysfunction-associated steatohepatitis (MASH), liver sinusoidal endothelial cells (LSECs) acquire a proinflammatory phenotype termed lipotoxic endotheliopathy. We previously identified glycogen synthase kinase 3β (GSK3β) as a central signaling hub in LSECs during MASH. To elucidate the molecular mechanisms and functional outcome of lipotoxicity-induced GSK3β activation in LSECs, we utilized endothelial cell-specific Gsk3β knockout (Gsk3β△End) mice fed MASH-inducing diets. Endothelial Gsk3β deletion significantly reduced markers of lipotoxic endotheliopathy, including adhesion molecules and chemokines, alongside liver injury, inflammation, and fibrosis. Immune profiling via flow cytometry and mass cytometry by time of flight (CyTOF) identified decreased hepatic infiltration of proinflammatory myeloid populations, particularly mature dendritic cells (DCs) in Gsk3β△End mice. In a co-culture system, GSK3β in lipotoxic LSECs promoted DCs maturation. Mechanistically, GSK3 inhibition restored lipotoxicity-induced alterations in LSEC mitochondrial morphology and respiration by regulating AMP-activated protein kinase and dynamin-related protein 1. This rescue suppressed chemokines and adhesion molecules expression, thereby limiting immune cell recruitment. Collectively, under lipotoxic stress, GSK3β amplifies mitochondrial dysfunction and inflammatory signaling in LSECs, enhancing myeloid cell homing and DC maturation. Targeting LSEC GSK3β may therefore represent a promising therapeutic strategy to mitigate LSEC driven fibro inflammatory response in human MASH.
Authors
Akitoshi Sano, Qianqian Guo, Khaled Warasnhe, Chady Meroueh, Nantawat Satthawiwat, Asma Hamdi, Ghefar Hmaydoosh, Xin Dai, Usman Yaqoob, Kevin D. Pavelko, Charlene Miciano, Tatiana Kisseleva, Zeba Firdaus, Patrick P. Starlinger, David Pereyra, Enis Kostallari, Petra Hirsova, Davide Povero, Samar H. Ibrahim
Abstract
Abdominal aortic aneurysm (AAA) lacks effective pharmacological therapies. Here, we investigate transcription factor 7-like 2 (TCF7L2), a genetic locus associated with both thoracic and abdominal aortic aneurysms, to elucidate its role in AAA pathogenesis. Integrating summary-data-based Mendelian randomization (SMR) with single-cell RNA sequencing (scRNA-seq) of human and mouse aortas, we identify TCF7L2 as a gene enriched in vascular smooth muscle cells (VSMCs) and causally linked to AAA development. Smooth muscle cell-specific TCF7L2 knockout significantly attenuates AAA formation across three distinct murine models (Ang II infusion-, BAPN/Ang II co-administration-, and elastase-induced AAA), independent of systemic blood pressure or lipid levels. Mechanistic studies reveal that TCF7L2 directly upregulates MMP14 and downregulates TIMP3 expression in vitro and in vivo, driving MMP2-mediated extracellular matrix (ECM) degradation. Concurrently, TCF7L2 represses integrin β1 (ITGB1) expression, reducing VSMC adhesion to the ECM. Collectively, these findings identify TCF7L2 as a key driver of pathological vascular remodeling in AAA, suggesting that targeting TCF7L2 may offer a novel therapeutic strategy for limiting AAA progression.
Authors
Yongjie Deng, Yaozhong Liu, Yang Zhao, Hongyu Liu, Guizhen Zhao, Zhenguo Wang, Xu Zhang, Chao Xue, Wei Huang, Tianqing Zhu, Haocheng Lu, Yanhong Guo, Lin Chang, Ida Surakka, Y. Eugene Chen, Jifeng Zhang
Abstract
Aortic dissection or rupture is a leading cause of mortality in vascular Ehlers-Danlos syndrome (VEDS), a disorder caused by mutations in the COL3A1 gene. Col3a1G938D/+ mice recapitulate features of VEDS, including high risk of aortic rupture. As in people with VEDS, aortic risk in this model accelerates at the onset of puberty, especially in males. We identify developmentally regulated gene programs associated with this vulnerability and that are targeted by treatments that mitigate aortic risk. Both genetic and pharmacological inhibition of the androgen receptor (AR) eliminated survival differences between sexes, while treatment with a dual AR and mineralocorticoid receptor (MR) antagonist provided near-complete and durable protection in both sexes. Pathways targeted by dual AR/MR inhibition, including those related to extracellular matrix (ECM) organization and cell-ECM interactions, largely overlapped with those also modulated by isolated MR antagonism. Selective targeting of MR signaling emerged as an effective therapeutic strategy in both sexes that avoids sexual side effects in males.
Authors
Emily E. Juzwiak, Caitlin J. Bowen, Rhiannon Edwards, Leda Restrepo, Serena Lee, Cassie A. Parks, Anthony Zeng, Maya M. Black, Oscar E. Reyes Gaido, Emily E. Bramel, Dustin T. Shigaki, Michael A. Beer, Chiara Bellini, Harry C. Dietz, Elena Gallo MacFarlane
Abstract
Pulmonary fibrosis is frequently accompanied by pulmonary hypertension, which can occur disproportionate to the extent of fibrosis, suggesting a fibrosis-independent vascular remodeling process. Here, we demonstrated that plasma growth differentiation factor 15 (GDF15) is elevated across diverse fibrotic lung disease subtypes and correlates with markers of elevated right heart pressures, but not pulmonary function indices, indicating a possible link to endothelial cell dysfunction. To investigate the import of endothelial GDF15 as a modifier of lung fibrosis pathogenesis, we generated endothelial cell-specific Gdf15 knockout mice, which showed protection from bleomycin-induced lung injury and fibrosis, with preserved lung function. RNA sequencing of human pulmonary microvascular endothelial cells revealed altered expression of barrier-regulatory genes in GDF15-deficient endothelial cells compared to controls. Functional studies confirmed that GDF15 knockdown attenuates thrombin-induced barrier disruption by reducing cytosolic Ca2+ responses. Together, these findings implicate endothelial GDF15 as a modifier of vascular permeability and Ca2+ signaling, and a contributor to lung injury and fibrosis.
Authors
Kristen Raffensperger, Marta Bueno, Brian J. Philips, Megan Miller, Máté Katona, Shuai Yuan, Adriana Estrada-Bernal, Byron Chuan, Pavan Suresh, Stephanie Taiclet, Scott Hahn, Yingze Zhang, Jonathan K. Alder, Seyed Mehdi Nouraie, Daniel J. Kass, Oliver Eickelberg, Adam C. Straub
Abstract
Aortic dissection (AD) is a catastrophic vascular emergency with high mortality, and current pharmacologic interventions to prevent its progression are limited. Vascular smooth muscle cells (VSMCs) undergo a pathological phenotypic switch from a contractile to a synthetic state during AD, compromising aortic wall integrity; however, the underlying metabolic mechanisms remain poorly understood. In this study, we performed integrative transcriptomic analyses and identified glutaminase 1 (GLS1) as a key regulator of VSMC phenotypic switching in AD. GLS1 expression was significantly downregulated in VSMCs from both human AD aortic tissues and mouse models. Functionally, GLS1 deficiency promoted PDGF-BB–induced VSMC dedifferentiation in vitro. Smooth muscle cells specific Gls1 knockout (Gls1SMKO) mice exhibited aggravated AD upon BAPN treatment, whereas VSMCs specific GLS1 overexpression improved the contractile phenotype and reduced AD incidence. Mechanistically, GLS1 downregulation impaired glutamate metabolism, leading to reduced levels of glutathione and α-ketoglutarate. This metabolic disruption promoted reactive oxygen species accumulation and mitochondrial dysfunction, ultimately triggering VSMC phenotypic switching. Furthermore, we found that GLS1 transcription was repressed by retinoic acid receptor-α (RARα). Pharmacologic inhibition of RARα with AR7 restored GLS1 expression, ameliorated VSMC phenotypic switching, and conferred protection against AD. These findings reveal a critical role of GLS1-mediated glutamate metabolism in VSMC phenotypic switching and suggest a promising therapeutic strategy for AD.
Authors
Wei Xie, Chen Ning, Chen Lu, Dongjin Wang, Shuang Zhao, Tianyu Song, Hailong Cao
Abstract
Chronic hyperglycemia induces microvascular complications in patients with type 2 diabetes (T2D), particularly diabetic retinopathy, nephropathy, and neuropathy. We revisited to examine such vascular damage in the pancreas in 3D. Using thick pancreatic tissue slices, we analyzed volumetric intraislet and peri-islet exocrine capillary density (vICD and vECD), as well as interface capillary counts along the islet periphery to quantify vascular integration between the islets and surrounding acinar cells. Contrary to the previous reports, vICD was not homogeneous, but highly heterogeneous across the five species studied (human, monkey, pig, ferret and mouse), especially in smaller islets (15%–80%). vICD became less variable with increasing islet size converging at approximately 20%. With this foundation of islet vascularization, pancreatic tissues from non-diabetic (ND) and T2D subjects consisting of eight age- and sex-matched pairs (age range of 35-65 years with various duration: 0-15 years) were examined. Strikingly, no significant differences in microvasculature were found, where mean vICD (~30%) and mean vECD (~15%) were nearly equivalent between the groups. Capillary integration with respect to islet size was comparable. It suggests that integrated pancreatic blood flow with robust crosstalk between the endocrine and exocrine pancreas may facilitate microvascular preservation in T2D via local distribution of insulin.
Authors
Alex M. Tollefson, Frank R. Marsico, Manami Hara
Abstract
We generated a comparative spatial proteomic atlas of the human and mouse retina using a highly multiplexed immunohistochemistry technique called iterative bleaching extends multiplexity (IBEX). We refined the IBEX workflow by integrating an antibody dissociation option alongside chemical bleaching. This dual strategy enabled removal of the entire antibody complex, permitting the flexible use of antibodies from the same host species across iterative cycles. We coupled this workflow with super-resolution imaging via deconvolution and applied it to the retina of healthy humans and WT mice and the Crb1rd8 mouse model. We successfully imaged over 25 protein markers on human and mouse tissue sections, generating spatial atlases of the major retinal cell populations. Cross-species protein expression was compared to scRNA-seq datasets to identify protein and transcript disparities. Super-resolution IBEX delineated the ultrastructural features of the outer limiting membrane (OLM), identifying CD44 as a core structural component tightly colocalized with a highly organized F-actin belt within Müller glial endfeet. Using the Crb1rd8 mouse model, disruption of this complex was spatially associated with rosette formation and OLM structural failure. In summary, spatial proteomic atlases of the human and mouse retina were used to reveal insights into the arrangement of major retinal cell populations and OLM structure.
Authors
Yuxuan Meng, Jakub Kubiak, Zuzanna Dzieniak, Lorna Fowler, Rose Avient, Jason Hopley, Linyulong Li, Chaoran Li, Yuan Tian, Bruno Charbit, Colin J. Chu
No posts were found with this tag.